Mobile medicine
Voice commands instead of floored pedals and wailing sirens – the first ambulances were drawn by horses. Later, the internal combustion engine replaced the horse as the power source. Technological progress spawned further ideas: In 1938, Martin Kirchner, a professor of surgery in Heidelberg, in an essay titled “The Mobile Surgical Hospital” said that pre-clinical medical treatment could save more patients. Theoretically true but, unfortunately, not feasible back then. Today, ECGs, defibrillators and respirators are standard ambulance equipment. On board of helicopters, ambulances have long conquered the skies as well.

Kirschner’s vision of a “mobile surgical hospital” has also long become a reality. For instance, as early as in 2008, a hospital on wheels made in Germany consisting of three Mercedes buses was delivered to the Centre of Ambulance Services in Dubai. Such mobile medical centers are deployed to the scenes of major incidents, such as accidents or catastrophes with many casualties, to provide fast on-site medical assistance. The centerpiece of the high-tech mobile hospital in Dubai is an intensive care unit including a fully functional operating room that’s integrated in one of the buses.
“The Future of Mobility will transform health care delivery, accelerating the use of distributed care models and changing where new facilities are built and how they are designed.”
From Deloitte’s document “Mobility will change the future of health care”
Mobile CT scanners in truck trailers or ORs in containers have been gaining traction too. Such mobile units help compensate for capacity shortfalls in hospitals, for instance during modernization projects. Such projects are rolled out clearly more often than they used to be 50 years ago because, due to accelerated technical progress, the service life of an OR has shrunk to between 10 and 15 from the previous 30 to 35 years. Mobile units help sustain hospital operations.
Mobile Medicine 4.0: Clinic on wheels summons itself
So much for the current state. By now, visionary brains of various research and development disciplines are working on Mobile Medicine 4.0, focused less on mobile intensive care units of the kind in Dubai but mainly on diagnostic and medication-related areas. “Mobile” in this context doesn’t necessarily mean “vehicle.” Smartphones and wearables, that is applications that are integrated in clothing etc., are becoming increasingly important mobile components of modern healthcare.
Artefact, an American technology design agency, has this vision of such a comprehensive medical use case: Using various ambient sensors distributed in areas such as a home or office, wearables or connections with the Internet of Things, a smartphone constantly collects health-related data. When values of concern are measured the system can summon a mobile, self-driving clinic. This uncrewed mobile clinic has further diagnostic equipment on board. Using augmented reality for a visual projection of their body, patients can pinpoint the location of their health issues to complement verbal descriptions. Based on all parameters, an artificial intelligence then provides a diagnosis and recommends an appropriate therapy. Ideally, the system’s on-board pharmacy can dispense the required medication. Should a real physician be needed, they can be included by video conferencing.

Many diagnostic and monitoring functions can also be integrated into other vehicles – combining the daily commute to and from the office with a routine checkup. However, a question not to be ignored in this regard is whether people are going to approve of such permanent physical monitoring and the related sharing of data. But then again, aren’t many of us already tracking physical performance indicators using a fitness app?
AI delivers better diagnoses than assumed
Another question that’s crucial not only for the previously described mobile use case is whether an AI will be able to truly replace a real physician in the future. In some areas, AI is already on an equal footing with human doctors. Especially in diagnostics, when it comes to matching an existing symptom with other cases and drawing conclusions from such comparisons, artificial intelligence systems have delivered better results in some tests than real physicians, for instance in skin cancer screening. Since a well “trained” AI accesses hundreds of thousands if not millions of comparison data items that’s not surprising. So, why shouldn’t we stand inside a mobile box during our lunch break and have our body scanned instead of waiting for months to see a specialist?
Mobility connects medicine with people
That, precisely, is the major benefit of mobile medicine: It delivers healthcare to people including those who normally don’t have access to it. Or to people who neglect having checkups due to lack of time or plain laziness. “In the individual case, this can mean that people suffer while unable to find a means to get to a medical expert and their ailment can progress beyond the point of using simpler methods to solve their health problem,” writes Dr. Lance B. Eliot, a specialist in AI and machine learning, in an article about mobile medicine in “Forbes” magazine. From a macroeconomic perspective, he continues that “In the aggregate, this means that as a society we are inadvertently increasing our costs of healthcare since we aren’t catching health issues early and thus having to pony up more medical care and more expensive medical care once the health issue finally starts to get resolved.” Hence investments in mobile healthcare applications can pay off not only in a humanitarian sense but also financially.
Flying Doctors
Air rescue using so-called multicopters – vertical take-off and landing aircraft propelled by several electric rotors – is possible, makes sense and improves emergency medical care of the population: In a nutshell, those are the results of the world’s first feasibility study on the use of these new aircraft that was commissioned in 2018 by the German Automobile Club ADAC. ADAC expressly states that multicopters are not intended to replace rescue helicopters but to complement their fast assistance from the air. Initially, multicopters are not planned to transport patients.
29 %
of all Africans live two or more hours away from a hospital, according to a study by the World Economic Forum. However, mobile services can massively improve healthcare not only in Africa but also in other rural areas without adequate medical infrastructure.
In an operating radius starting at 25 kilometers (16 miles), multicopters flying at a speed of up to 150 km/h (93 mph) can take emergency physicians to the scene of an emergency faster than ground-bound ambulances having to fight their way through urban traffic. Because average arrival times of emergency physicians in Germany have increased by almost 40 percent in the last 20 years, this is an important advantage. Another one is that emergency physicians can work more effectively and the multicopter can adequately mitigate the lack of emergency physicians existing in many areas. As a third benefit, the positive image of rescue missions can help increase public acceptance of multicopters as a new means of mobility.

Delivering healthcare to people: That’s the approach that by now has been driving more than 2,000 mobile clinics through the United States, where they’ve become a pillar of the healthcare system. Besides residents of rural areas, low-income earners, homeless people, and those without health insurance particularly use this mobile medical service. In Germany, so-called Medibuses have been traveling through big cities like Berlin and Hamburg since summer of 2022. The vehicles have equipment like a complete doctor’s office and are intended to provide medical assistance primarily to refugees as well as poor people in their immediate living environment. If necessary, the teams can access medically trained video interpreters for several languages and other resources. There are many reasons for deploying such a service: They include shortages in specialist medical care as well as language barriers and lack of information and guidance pertaining to the legal and health systems. As a fast mobile task force, the Medibus teams circumvent such hurdles with their unbureaucratic services. After all, the best physicians are of no use if they’re not accessible.
Schaeffler puts medicine in motion
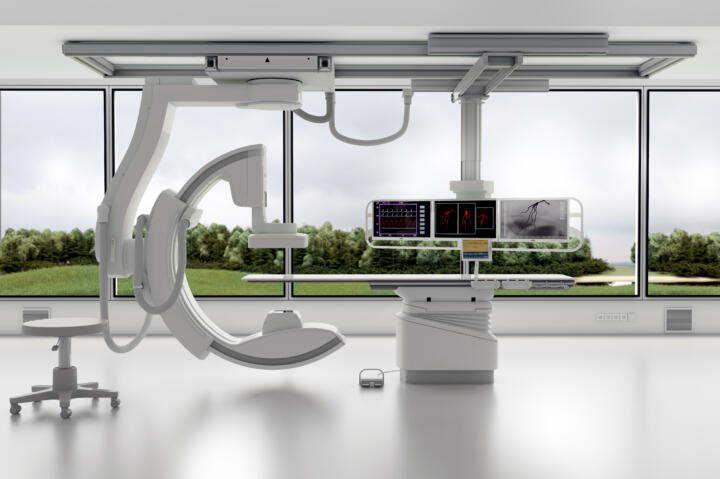
With its Industrial division, the supplier has been active also in the medical device technology sector for many years. Components from Schaeffler are used particularly in medical imaging such as C-arms, X-ray tubes and CT scanners.
“Leading equipment manufacturers rely on our low-noise CT bearings and drive systems to achieve high levels of scanning quality, for example,” says Ralf Moseberg, Senior Vice President Industrial Automation at Schaeffler. In the OR area, especially in ceiling-mounted swivel arms, Schaeffler products are used as well: rotary bearings, brakes and, again, drive units. Moseberg: “No matter where linear and rotary guides up to and including robotics applications are used in healthcare settings, you’ll almost always find our motors, gearboxes or even complete kinematic systems.” Medical device technology is a strategic growth field for Schaeffler. The company intends to significantly grow its business in that sector and make it one of the key pillars in the Industrials market. Moseberg and his colleagues also emphasize in-house mobility in that regard: CT scanners using drive systems from Schaeffler can be moved quickly from one room into another one, which increases patient throughput and enhances treatment efficiency. The recently announced acquisition of linear technology specialist Ewellix underscores Schaeffler’s ambitions. Ewellix is one of the market leaders in the field of electromechanical industrial actuators, lifting columns and planetary roller screws, among other things. In addition to robotics and mobile machines, they’re used primarily in medical device technology – in dental medicine, care for preterm and newborn babies or in surgical as well as in rehabilitation and fitness equipment.